Welcome to the Wonderful World of Wizzys
So what are we going to do about impacted wisdom teeth in a world without dentists? Not to put too fine a point on it…Suffer. Let me explain.
God felt that humans needed 32 teeth to function together and support each other for a lifetime. As a creationist, I believe that before Eve gave Adam the apple and he ate it, that this was true. However when sin entered the world, conditions changed, and all living things were subject to deterioration of their genetic code. These mutations were passed on generation to generation, with each new stage adding its own mutations to the mix. One of the human consequences has been the imbalance of the total width of the teeth exceeding the amount of space in the dental arch. In some people, we see the effects of this by crowding of the teeth (and the orthodontist gets another job); in others, there is no room for all the teeth and the last ones never erupt fully into the mouth (and the oral surgeon gets another job).
Our evolutionist friends explain this phenomenon as the result of natural selection modifying the jaws to account for modern diet, where food is softer and therefore less mastication is needed. OK, if you say so. I have seen photos of skulls of Anastasi Indians that are carbon dated to c. 3000 BC, they did not have a modern diet…they did have impacted wisdom teeth, go figure.
Regardless of the origin of the problem, the symptoms and underlying causation must be dealt with. Most wisdom teeth related emergency issues in the dental office come from a condition called pericornitis. This occurs when bacteria is introduced into the pocket around the crown of the semi-erupted lower wisdom tooth. Bacteria and associated toxins lead to irritation and swelling. The swollen tissue gets pinched between the upper and lower teeth. This can be very uncomfortable and lead to the patient keeping their jaw in an eccentric position to avoid the pinch, which leads to chronic muscle stress and associated pain. This infection can in and of itself lead to fever and a sore throat. Another consequence can be trismus, where the masseter muscle goes into spasm limiting jaw opening to about an inch. This problem seems to be unique to third molars. I do not see it during the eruption of the other molars, even though they sometimes come in in a similar manner.
So what will we do if the dentist and his panoramic x-ray machine are no longer in business? Well, as with every other treatment, we have to make keen observation and act to minimize or eliminate the causative factors. If there is significant swelling and trismus, we have to use warm salt water rinses and possibly antibiotics, if available, to get us past the crisis. Aspirin or ibuprofen will help with pain and inflammation. Assuming that we can see the area, first we need to begin the process of flushing the pocket of tissue that the tooth is contained in. In my practice, I use 0.12% chlorhexidine rinse (Peridex) for this purpose. One could also use warm salt water, hydrogen peroxide, Listerine, or some other reasonable consumable liquid. I use a 5cc syringe that has a curved tip, but one could use any syringe with a needle with the tip cut off, smoothed and bent to fit. The process is to run the tip under the tissue fold as far as can be tolerated and then flush the pocket to remove bacteria and debris as well as oxygenate the area. Do not inject the tissue, just flush the pocket. This may need to be done several times over a day or two, until the acute phase of the pericornitis is resolved. At some point, it may be necessary to remove the tooth above or below the tissue if there is a significant pinching of the tissue that will not let the swelling go down.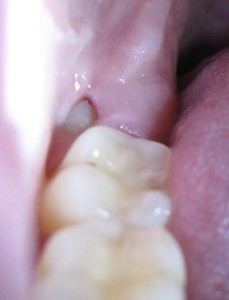
Once the acute inflammation is resolved, one needs to evaluate the actual wizzy involved. Without an x-ray, it is problematic to guess at the condition of the whole tooth from the portion of the tooth that you can see. If you have a good grasp of dental anatomy, sometimes a small portion of tooth exposed is enough to deduce the lay of the underlying whole. Believe me when I say that removing anything more complex than vertical and in line with the other teeth is beyond the scope of a neophyte. (I will post a Pro’s only addendum to this for further instructions.)
If no professional help is available, it will be necessary to continue the flushing once or twice a day indefinitely. Only if this is in a teenager is there any real hope that further growth and maturity may resolve the condition. This may be one of those things that will just need to be tolerated in the hard times ahead.
Copyright © 2011 WH2THDR
Related articles
- The Dreaded Question . . . (armageddonmedicine.net)
- Abscessed Teeth – Where will they lead? (armageddonmedicine.net)



I also am an OMF surgeon and concur with wh2thdr’s comments, including his last paragraph of July 19th post. I just requested a professional’s password and look forward to viewing his pw-protected post.
In extreme situations, might it not be possible to make a small incision to the gum and, with appropriate care, allow the tooth to emerge? Or, in the alternative, cut away the soft tissue and elevate the tooth out entirely?
{I’ve forwarded the question to the author of the article . . . I don’t know the answer myself. Any other dentists care to comment? – Doc Cindy}
Ohgoodgrief is on the right track, the second part of your post is called extraction, and ipso facto ends the problem. The first part is possible under rare circumstances but….
If we are dealing with an eruption issue, then the incision idea might be efficacious. Usually your pericoronal wizzy (wisdom tooth) is impacted and is in (erupted) as far as they are going to come, due to getting caught on the teeth in front of them. Also, so often this tissue is very inflamed and swollen. I may be over cautious, but I do not find that I have predictable results with surgery under these conditions. Finally, there is a natural lay or drape of the tissue in the wizzy area. Almost always alteration to the anatomy there is temporary and with in a short time there will be a rebound to the original condition.
Every situation is different, and, as practitioner, you have to make the call. I can remember only a couple of times, since dirt was invented, that I have done a “plasty” of the pericoronal tissue with what I would call good success.
wh2thdr