On 9/23/10 Concerned said: Any advice for a 40 something RA patient on Rituxan?
The cost for Rituxan, a drug used for both cancer patients and rheumatoid arthritis, is approximately $665/bottle, making it unlikely that stockpiling the drug is a viable option. Stability of the drug is another issue, as it comes in liquid form and requires refrigeration. Additionally, it’s not a medication most primary physicians are familiar with, and so monitoring treatment is a problem as well.
In the event of Armageddon or TEOTWAWKI resorting to non-steroidal anti-inflammatory drugs, pain meds, and steroids is almost a certainty. Although steroids have long-term side-effects, I expect that would be a secondary concern when the survival of the world is at stake. But at least prednisone and other steroids are dirt-cheap, readily available, and likely to remain stable in the original packaging for a number of years.
My advice is to talk to your doctor about other options, maybe not for now, but just in case. I don’t know your degree of arthritis, or whether the medicine is for comfort or life-saving, but it’s a legitimate question to ask, “If I couldn’t get this drug, how do you think I’d be if I had to take steroids?” In a future blog I’ll address the rational use of steroids for acute and chronic illness when other options are unavailable.
The remainder of this article is excerpted from my other blog at www.101waystosavemoneyonhealthcare.info.
People suffering from rheumatoid arthritis often exhibit findings displayed in the pictures below.

- Image via Wikipedia
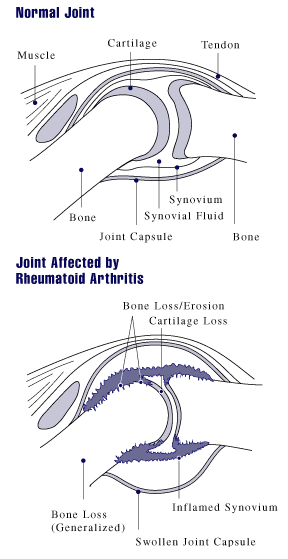
- Image via Wikipedia
Treatment of RA involves relieving symptoms and sometimes preventing further destruction of the affected joints.
In the early stages, RA is often managed like OA (osteoarthritis). If you have RA and your symptoms improve with a non-steroidal anti-inflammatory drug (NSAID), then that is usually the medication of choice.
Among the NSAID class of drugs, there are several available for only $4/month (ibuprofen, naproxen, diclofenac, others). Although many patients are prescribed the more expensive Celebrex (for $120 more), in general, it doesn’t actually work any better than the others. In fact, many of my patients say simple aspirin works best.
If doctors can treat a problem for $4 a month, why would we use a drug that costs over $100? The prime reason is actual or anticipated side-effects. All of the NSAID drugs have a tendency to irritate the stomach lining, occasionally causing ulcers. This may lead to GI bleeding and anemia (and even death). Celebrex was specifically designed to decrease (but not eliminate) the likelihood that this problem will occur. In some patients it makes a remarkable difference which NSAID is used. In other patients it seems to make little difference.
Until Celebrex came along, patients who required an NSAID but had gastric (stomach) irritation as a side-effect were often treated with an acid-lowering stomach medicine such as Prilosec, Prevacid, or Nexium. Before those 3 drugs were on the market we used the older acid-lowering drugs: Zantac, Tagamet, Axid, and Pepcid. However, when these stomach meds cost over $100 themselves, it made little sense to replace one expensive medication with another.
Now though, several of the stomach medications are available as generic, some for as little as $4/month. Self-pay patients and those with high co-pays on brand-name medications may want to consider using a $4 NSAID and a $4 stomach medication in place of the $100+ Celebrex.
Another cost-saving consideration for RA relates to blood testing. Unlike osteoarthritis, RA often shows up in the blood with a positive rheumatoid factor assay, elevated sed rate, or high ANA. Although I find these blood tests useful for diagnostic purposes, once the diagnosis has been firmly established, I have not found them very useful in monitoring the progress of the disease. Other doctors may disagree, but if repeating these blood tests does nothing to change the therapeutic plan, then why repeat them at all? The results are not very closely aligned with the degree of symptoms.
Patients with moderate to severe RA may be prescribed a disease-modifying agent such as Humira. A two-vial box of Humira costs $1799.81 at drugstore.com. Who can afford that much a month? And that’s just the beginning. Lab tests and frequent doctor visits add to the expense. So far, the only patients of mine who have taken this drug are those with excellent prescription coverage, i.e. – someone else is paying. Not a one of them has told me that they would consider taking this drug if they were paying for it themselves.
I have yet to see a patient with a remarkably good response (though there must be some somewhere). How do we measure how much improvement a patient should get in order to justify $20,000 a year for medication? I’d say, quite a bit.
And it’s a fallacy to simply think, well, someone else is paying. You’re paying, I’m paying, we’re all paying. If there are doctors out there who have found these expensive medications to be life-changing, I’d like to hear from you. I have not been impressed with what I’ve seen to date.
Of course, the pharmaceutical company does offer their drug for free or at a reduced price to those who cannot afford it (but does that mean everyone else is paying even more?)
Doctors prescribe these drugs because they sometimes help. According to the American Family Physician Cochrane analysis of benefit (Am Fam Physician. 2006 Feb 1;73(3):435, online at: http://www.aafp.org/afp/2006/0201/p435.html ) between 2 and 13 patients must be treated with Humira to demonstrate a significant response in only 1. So instead of costing $20,000 to do some good, it could be $200,000 instead, spread out over a number of individuals whom it hasn’t helped at all. Maybe I’m just a penny-pincher, but is there an element of craziness here?
Though I cannot solve this problem for the world, here is another tidbit of good advice for arthritic patients: get plenty of sleep. It helps your body recover from the effects of gravity. That’s my plan for the next 8 hours.
Image by pollyalida via Flickr
© Cynthia J Koelker, MD – All rights reserved
http://www.101waystosavemoneyonhealthcare.com/
Related articles by Zemanta
- Rheumatoid arthritis – All Information (umm.edu)
- Arthritis – All Information (umm.edu)
- New Drug Helps Treatment-Resistant Arthritis (arthritis.webmd.com)




As a young mother who has suffered with debilitating RA symptoms for years, Humira has changed my life. Gravity has nothing to do with eleviating the wrath of an autoimmune disease, so to suggest more rest is not only insulting but idiotic.
[Thanks for writing, Jennifer. There certainly are manifestations of an autoimmune arthritis that are not gravity-related, in particular vascular and other extra-articular disease. For these patients, rest is unlikely to help sufficiently, though again, rest does help relieve pain in weight-bearing joints. I’ve known a few RA patients who suffered autoamputation of fingers and toes along with end-stage renal disease. Happily, most patients with RA are not severely affected. Regarding treatment, unfortunately, Humira is not likely to be an option at TEOTWAWKI. While systemic steroids are not ideal, they do provide an inexpensive (and hopefully available) alternative to the biologic agents. The bisphosphonates help prevent steroid-induced osteoporosis to a degree, and with alendronate now available for $9/month, at TEOTWAWKI steroids+alendronate are a viable option – especially if the goal is to survive. In countries where people are commonly infected with parasitic nematode worms RA and other autoimmune diseases are rare. Perhaps voluntary worm infestation will become the preferred treatment of rheumatoid arthritis once modern biologic agents become unavailable. Let’s hope that never occurs. – Doc Cindy]
I take methotrexate, and am very concerned about the “taper” required to stop taking the drug. In the worst situation, what must I do to avoid/alleviate side effects as I try to switch to just Prednisone and OTC drugs? I only get my 7 x 2.5 mg pills in a 12 week supply.
Thanks!
[Doc Cindy replies: not knowing your situation, the answer may be more complicated than this, but in my rheumatoid patients I have not had a problem switching directly from methotrexate to prednisone without a methotrexate taper. I’d probably aim for a bit higher dose of prednisone to start with than a maintenance dose would be. Any rheumatologists out there are invited to reply as well. Methotrexate is not a drug most docs would write long-term supplies of, since periodic blood monitoring is required, though at low doses, problems are uncommon.]
My husband take methotrexate and it works very well for him.
At the end of the world as we know it, therapy with methotrexate will be a problem if labs cannot be monitored regularly (kidney function, liver, function, blood count). It is effective for many inflammatory diseases, as well as certain cancers. The possible benefit would have to outweigh the risk. I imagine NSAIDs and steroids would become the therapy of choice for most patients with RA.