Could you diagnose anthrax on your own? How about gonorrhea? A Gram stain is often diagnostic, and can be performed with limited equipment.
The following post on clinical laboratory procedures is contributed by Pete Farmer, who holds advanced degrees in research biology and history, and is also an RN and EMT. For Part I of the series, click HERE.
Thanks, Pete, for this timely article.
* * *
Images show sample Gram stains – What are they? – See key below.
* * *
Now that you understand the theory and practice of light microscopy at a more detailed level, as covered in the previous three installments of this series, it is time to perform a diagnostic staining technique.
The Gram stain is the most commonly-used differential staining technique in microbiology; it is named after its inventor, Danish scientist Hans Christen Gram (1853-1938), who published his findings in 1884. Though well over a century old, the Gram stain remains a key part of the clinical microbiologist’s repertoire. Before getting to the staining procedure, some background will prove helpful.
The hidden world of microorganisms is vast; it contains not only a staggering number of individual microbes – bacteria, viruses, protozoans, and fungi – but a huge number of individual taxonomic types and subtypes. The first scientists to study microbes, therefore, had the daunting task of somehow making sense of the sometimes-bewildering array of microscopic life forms. They began the painstaking task of classifying microbes on the basis of all sorts of criteria, from their appearance under the microscope to where they were found in the natural world to their chemical and physical characteristics. Bacteria can be classified depending on what kind of growth medium they prefer, i.e., the substrate upon which an organism grows or to which it is attached; the metabolic end-products they secrete into the surrounding environment; and much more. Bacteriologists began devising chemical and physical tests to allow typing of individual bacteria or groups of bacteria; over time, researchers learned when and how to use these tests to differentiate between microbes.
In 1923, “Bergey’s Manual of Determinative Bacteriology” was published for the first time; updated annually; it remains a standard reference for identifying bacteria. In brief, the manual uses a comprehensive battery of known characteristics of bacteria, organized into a decision-tree or algorithm, to separate microbes into the broad groups (or families) and then narrows the identification down to a single type of bacterium over the course of subsequent tests. Very often, when a scientist or clinician is confronted with a sample suspected or known to contain unidentified bacteria, his or her first action will be to perform a Gram stain. The Gram stain is often necessary but insufficient to complete an identification or diagnosis; that is, an investigator will have to perform other tests to make a definitive identification. However, in other cases, knowing the Gram stain result for a given bacterial sample is all the information a physician needs to make an informed decision about whether or not to prescribe an antibiotic and which one to use. Modern molecular biology and medical diagnostics labs have sophisticated gene-sequencing and similar methods which have supplanted differential staining, owing to their higher degree of specificity, greater precision and accuracy and lesser incidence of identification errors and cross-reactivity. However, the basic Gram stain remains a very useful adjunct to its more-modern counterparts, especially for diagnosis under harsh conditions where high tech methods may not be available.
The basis of the Gram stain lies in the differing cell wall composition among different types of bacteria. Some bacteria have thick, mesh-like cell walls rich in peptidoglycans (a chemical polymer consisting of amino acids and sugar); these bacteria, referred to as Gram positive (+), stain violet/purple in the procedure. Bacteria possessing a thinner peptidoglycan coating and an endotoxin (lipopolysaccharide) layer, referred to as Gram negative (-), stain red-to-pink.
Note: before proceeding, assemble the necessary supplies, chemical reagents, jars, slides, and other materials necessary to perform a Gram stain, as detailed in previous installments of this series, and according to the many published descriptions of the procedure. If making your own stain and counter-stain is too difficult or time-consuming, gram staining kits and reagents may be purchased premanufactured.
The following procedure is taken from the website, “Microbial Life Education Resources,” (http://serc.carleton.edu/microbelife/research_methods/microscopy/gramstain.html). This useful resource includes a short video clip of a Gram stain being done.
Gram stain protocol
Reagents: Crystal violet (primary stain), Iodine solution/Gram’s Iodine (mordant that fixes crystal violet to cell wall), Decolorizer (e.g. ethanol), Safranin (secondary stain), Water (preferably in a squirt bottle)
- Make a slide of cell sample to be stained. Heat fix the sample to the slide by carefully passing the slide with a drop or small piece of sample on it through a Bunsen burner three times.
- Add the primary stain (crystal violet) to the sample/slide and incubate for 1 minute. Rinse slide with a gentle stream of water for a maximum of 5 seconds to remove unbound crystal violet.
- Add Gram’s iodine for 1 minute- this is a mordant, or an agent that fixes the crystal violet to the bacterial cell wall.
- Rinse sample/slide with acetone or alcohol for ~3 seconds and rinse with a gentle stream of water. The alcohol will decolorize the sample if it is Gram negative, removing the crystal violet. However, if the alcohol remains on the sample for too long, it may also decolorize Gram positive cells.
- Add the secondary stain, safranin, to the slide and incubate for 1 minute. Wash with a gentle stream of water for a maximum of 5 seconds. If the bacterium is Gram positive, it will retain the primary stain (crystal violet) and not take the secondary stain (safranin), causing it to look violet/purple under a microscope. If the bacterium is Gram negative, it will lose the primary stain and take the secondary stain, causing it to appear red when viewed under a microscope.
Bacteria are characterized in part by their morphology (structure and form). Cocci (singular = coccus) are spherical in form, and may appear in groups or two or more arranged in characteristic shapes. Paired spherical bacteria belong to the group (genus) Diplococci; the Streptococci are spherical and appear in chains; Staphylococci appear in large groups and may form distinct shapes. The causative agent of strep throat (Streptococcal pharyngitis) is a subtype of Streptococcal bacterial family known as the Group A beta-hemolytic Streptococcus. A second morphology is the bacillus (plural = bacilli) or rod-shaped bacterium. Escherichia coli is an example of a rod-shaped bacterial form. A third form is the spiral-shaped bacterium, or spirillum. Treponema pallidum, the causative agent of venereal disease syphilis, is an example of a spiral bacterial type.
Combined with morphology, the gram stain is a powerful tool for characterizing bacteria for diagnostic purposes. Six common gram positive bacteria that infect humans are the staphylococci, streptococci, bacilli, clostridia, corynebacteria, and listeria types. Examples of gram negative infectious agents which affect humans include the Spirochete and Neisseria types.
Copyright © 2011 Peter Farmer
IMAGE KEY
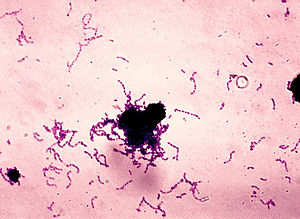
Top (large) image: anthrax in CSF fluid (purple rods)
Image #2, toward right: streptococcus mutans
Image #3, toward left: bordatella pertussis (causes whooping cough)
Image #4, toward right: gonococcus (note organisms within cells)





Will there be additional parts or is Part 4 the end?
Good series
Pete’s writing a series, and has more planned on practical labs. I hope to add to these (and anyone else is encouraged to contribute as well) after my book edits are done (which is taking all my extra time).
Thank you Pete Farmer for taking us all through the basics again.
This information will be invaluable for all medical officers to teach their assistants in preparation for on location diagnoses and treatment.
Do we have your permission to use this material for prep group presentations and as a teaching aid?